Table of content
Table of content
Most people don’t think about their jawbone at all. Why would they? You lose a tooth, you get used to it, and life goes on.
Then one day you start asking about an implant… and suddenly the dentist says, “You don’t have enough bone here.” And you hear things like “bone loss” or “we’ll need to build this area first,” and that’s usually when it starts to feel more complicated than you expected.
The truth is, implants need solid bone to stay in place. If that bone has slowly shrunk over time—which is pretty common after a tooth is missing—the implant just won’t have the support it needs. That’s why rebuilding bone is such a big part of implant treatment today.
And that’s also why some people now hear about stem cell therapy in dentistry. Not as something fancy or futuristic, but as a possible way to help the body rebuild jaw bone in harder cases.
So, the real questions become pretty simple: can stem cells actually help with bone growth? And do you really need something like this, or is it only for certain situations?
Why Bone Matters So Much for Implants
Here’s something most people don’t realize: an implant isn’t just “a tooth.” It’s more like a screw that has to sit inside your jaw and stay there for years while you chew, talk, and forget it even exists.
And that only works if the bone is actually there to hold it.
The annoying part? Bone disappears quietly. If a tooth has been missing for a long time, the bone under it slowly shrinks. You don’t feel it happening. You don’t see it. Everything seems fine… until you finally decide, “Okay, I want an implant,” and the scan shows there’s just not much bone left.
Things like gum disease, old infections, or extractions from years ago can make this worse. Sometimes the dentist isn’t even talking about the implant yet. They’re talking about fixing the foundation first.
Basically: no solid bone = no solid implant. Simple as that.
The Usual Solution: Bone Grafting
For many years, bone grafting has been the standard way to deal with this problem, and it’s the approach recommended in mainstream dental guidelines, including those from organizations like the American Dental Association (ADA).
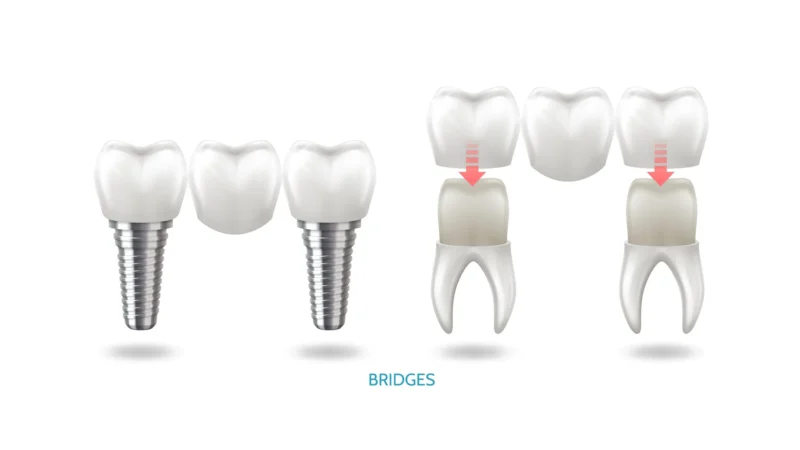
In simple terms, the dentist places a special bone material in the weak or missing area. Your body then slowly replaces that material with real bone over time. This material can come from:
- Your own bone
- Donor bone
- Or synthetic bone materials
And to be clear: this approach works. It’s used every day, all over the world, and it has a long track record.
But it also has some limits. Healing takes time—often several months. Sometimes more than one procedure is needed. And the final result depends a lot on how well your body heals. In more difficult cases, bone growth can be slow or less predictable.
Because of that, doctors started looking for ways to support the body’s healing process, not just fill space. That’s where stem cells enter the conversation.
So… What Are Stem Cells?
Stem cells are not as mysterious as they sound. Your body already has them. They’re just cells that haven’t “picked a job” yet. Depending on what your body needs, they can turn into things like bone, muscle, or cartilage.
In dentistry, when people mention stem cells, they’re usually talking about mesenchymal stem cells (MSCs). These are found in places like bone marrow or fat tissue, and their main role is pretty simple: help with repair.
hey can:
- Turn into bone-forming cells
- Help with tissue repair
- Send signals that support regeneration
It helps to think of them as helpers that encourage your body to rebuild itself more effectively.
How Stem Cells May Help Regrow Jaw Bone
Stem cells don’t just get injected and suddenly create new bone on their own. In real treatments, they’re usually used together with bone graft materials. The graft provides the structure. The stem cells help make the healing environment more active and more supportive for real bone growth.
They may help by:
- Turning into bone-forming cells
- Improving blood supply to the area
- Helping the graft integrate better with your own bone
- Supporting better-quality healing in more difficult cases
In some cases, this can also mean more predictable healing, and sometimes even a slightly faster healing process — though it’s never a guarantee and never a replacement for good surgery.
The goal is to improve healing in situations where healing is already challenging.
When Is This Actually Useful?
Honestly, most people don’t need this.
If your bone is in decent shape and your general health is good, traditional bone grafting usually works just fine.
Stem cell–supported regeneration is mainly considered in more complex cases, such as:
- Sinus lift procedures
- Severe bone loss
- Very thin jawbone ridges
- Old, long-standing missing teeth
- Areas where healing is expected to be slow or unpredictable
In other words, this isn’t for “everyone getting an implant.” It’s for cases where the body clearly needs extra help.
The Honest Pros and Cons
Possible upsides:
- More biologically active healing
- Better integration of graft materials
- Potentially better bone quality in difficult cases
Real-world limits:
- Higher cost
- Not available everywhere
- Still evolving medically
- Strict rules and regulations
- Not necessary for most patients
This isn’t a replacement for bone grafting. It’s a supportive tool for specific situations.
Safety, Rules, and Common Sense
Anything involving stem cells is medical treatment—not wellness, not cosmetics, and not a trend.
That means:
- It must follow strict medical standards
- It must be done under proper supervision
- It must comply with local laws and regulations
- And it must be based on real evidence, not marketing
A serious clinic will never sell this as a miracle solution. And it won’t use it when simpler, proven methods are enough.
Why Planning Still Matters More Than Any “Advanced” Technique
Here’s the part people sometimes forget: no biological technique can fix bad planning.
Long-term success still depends on:
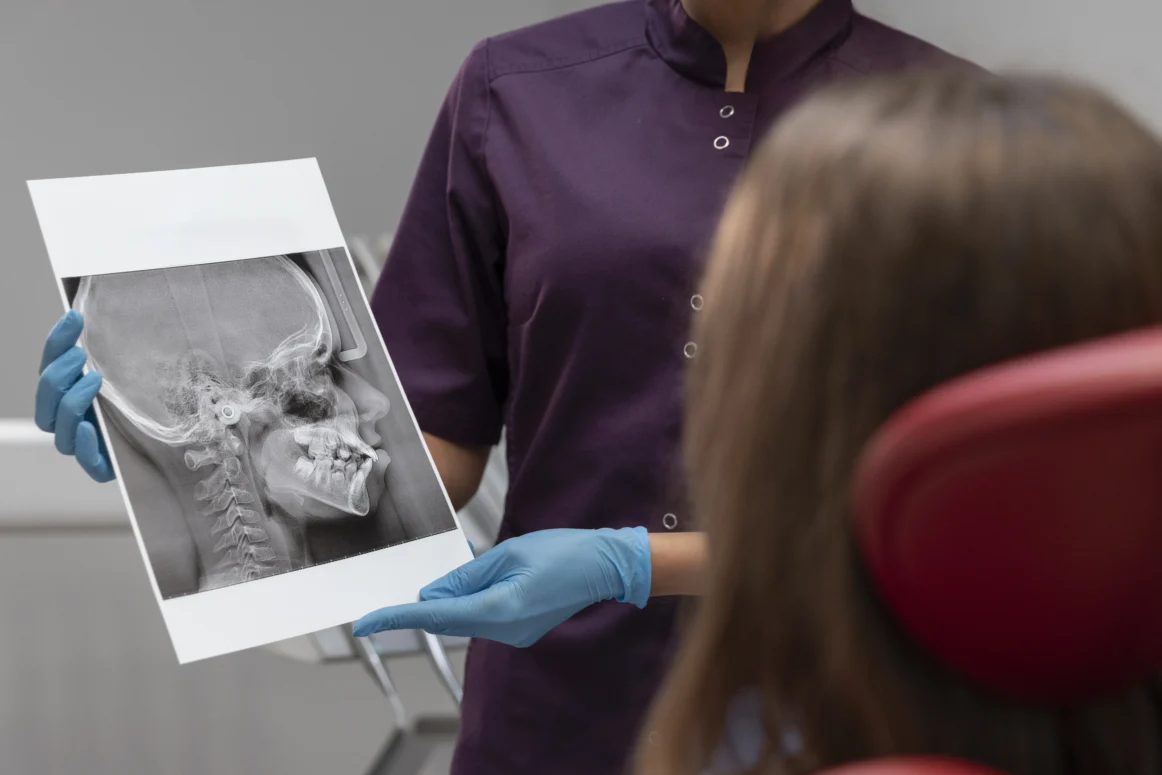
- Proper 3D scans
- Correct diagnosis
- Accurate surgical placement
- Good bite design
- And careful healing time
Stem cells can support healing. They can’t rescue poor dentistry.
Why Many Patients Look to Turkey for Complex Treatments
When people start dealing with bone loss and advanced implant planning, they often realize two things: it needs to be done properly, and it can get expensive.
That’s why many patients from Europe, the UK, and the US look at clinics in Turkey. Not because standards are lower—but because operating costs are lower, while technology and experience can be just as high.
For some, it also turns treatment into a planned trip instead of a stressful medical rush, giving them time to recover in a calmer setting.
Why Choose Dentspa for Bone Regeneration and Implants?
At Dentspa, treatments like bone regeneration aren’t treated as “extras.” They’re part of a proper medical plan
In practical terms, that means:
- Full 3D scans and bone analysis before decisions are made
- Digital planning for safe, accurate placement
- Evidence-based use of regenerative techniques
- High-quality materials and trusted systems
- Team planning for complex cases
- Clear scheduling and aftercare for international patients
The goal isn’t just to place an implant. It’s to make sure the bone underneath is strong enough to support it for years.
So… Can Stem Cells Really Help Regrow Jaw Bone?
In the right cases, with the right technique and the right planning, they can support real bone regeneration.
But they’re not magic. They’re not for everyone. And they’re not a shortcut.
For most people, standard grafting works perfectly well. Stem cell approaches are mainly for more difficult situations where healing needs extra biological support.
If you’ve been told you don’t have enough bone for implants, the best next step isn’t guessing—it’s proper imaging and honest advice.
At Dentspa, you can book a free consultation, review your scans with the doctor, and leave with a clear understanding of your options and what the next steps should be.
Frequently asked questions
Who is not a candidate for stem cell therapy?
Most people.
If your bone can be fixed with a normal graft, that’s usually what makes sense. Simple works. There’s no prize for making a treatment more complicated than it needs to be.
It’s also not a great idea if you have health issues that already make healing tricky. In those cases, dentists usually want fewer moving parts, not more.
So, this isn’t an “everyone should do it” thing. It’s more like a “maybe, in certain tough cases” thing. If someone is pushing it as the default option, that should make you pause.
Is stem cell dental treatment legal everywhere?
No, it isn’t. The rules are different from one country to another, and they’re still changing in many places.
In some countries, certain uses are allowed under strict medical conditions. In others, it’s limited or not permitted at all. That’s why any serious clinic has to follow local laws and medical guidelines very closely — and why you shouldn’t trust anyone who treats this like a trend or a loophole.
If a dentist offers this kind of treatment, they should be able to explain clearly what’s allowed where they practice, and why it makes sense in your specific case.
What are alternatives to bone grafting?
Sometimes there are other ways around a full bone graft. It depends on the case.
In some situations, dentists can use different types of graft materials, or guide the bone to heal in a certain way with special membranes and techniques. In more complex cases, there are also regenerative approaches that try to help the body rebuild bone more actively.
But here’s the honest part: none of these are “magic replacements” for good planning and proper surgery. They’re just different tools for different problems. The real decision always comes down to what your scans look like and what will actually be stable in your mouth long-term.
How long does bone regeneration take after a graft?
For a lot of people, it’s around 3–6 months before the bone is strong enough to work with. Sometimes less. Sometimes more. Bigger graft? Takes longer. Healing not great? Takes longer.
Sometimes your dentist just waits a bit extra to be safe, because stronger bone now saves problems later.
Is stem cell therapy for bone regeneration safe?
It can be safe. But only if it’s done properly, and in the right place.
This isn’t a beauty treatment or something you just “add on” because it sounds advanced. It’s real medical work. Safety depends on very practical things: where the stem cells come from, how they’re handled, and who’s actually using them. In a serious clinic, this means strict lab standards, clear protocols, and a clear medical reason for doing it in the first place.
Most problems don’t come from the idea of stem cells itself. They come from cutting corners. From poor planning. From places that don’t follow proper rules or don’t really explain why the treatment is being used.
That’s why a responsible dentist will only suggest this when it truly makes sense for your case — and only if it’s allowed and properly regulated where they work.
Can stem cells regrow jaw bone?
Short answer: sometimes they can help — but they’re not magic.
Stem cells don’t just get added and suddenly create new bone on their own. In real treatment, they’re usually used together with bone grafts and proper surgery. The graft gives the shape. The surgery puts everything in the right place. The stem cells just help your body do the healing part a bit better.
In the right kind of case — usually when bone healing is expected to be difficult — they can support real bone growth. In simple cases, though, most people don’t need them at all.
So, it’s less “stem cells regrow your jaw” and more “stem cells can help your body rebuild bone when it needs extra support.”













 70%
70% 

