Table of content
Table of content
Most people start researching dental implants the wrong way. They search for prices, find a big range, get confused, and either book the cheapest option or do nothing. Neither usually ends well.
What actually matters — before price, before clinic, before anything else — is understanding what you’re getting into and whether you’re even a candidate. That’s what this is about.
Why does the jawbone matter so much?
When a tooth is extracted and nothing replaces it, the bone underneath starts to disappear. Not dramatically, not overnight — but consistently. The jawbone maintains its density because tooth roots stimulate it every time you chew or bite. Remove the root, remove the signal. The bone resorbs.
In the first year after an extraction, measurable bone loss has already begun. By year two or three, patients who waited often need bone grafting before an implant is even possible — a procedure that adds months and cost to the whole process. We see this regularly at DentSpa. A patient who could have had a straightforward implant in one visit now needs two separate procedures and a longer recovery, simply because they assumed they had more time.
The decision isn’t really “implant or no implant.” It’s “implant now, or a more complicated version of the same thing later.”
What is a dental implant, actually?
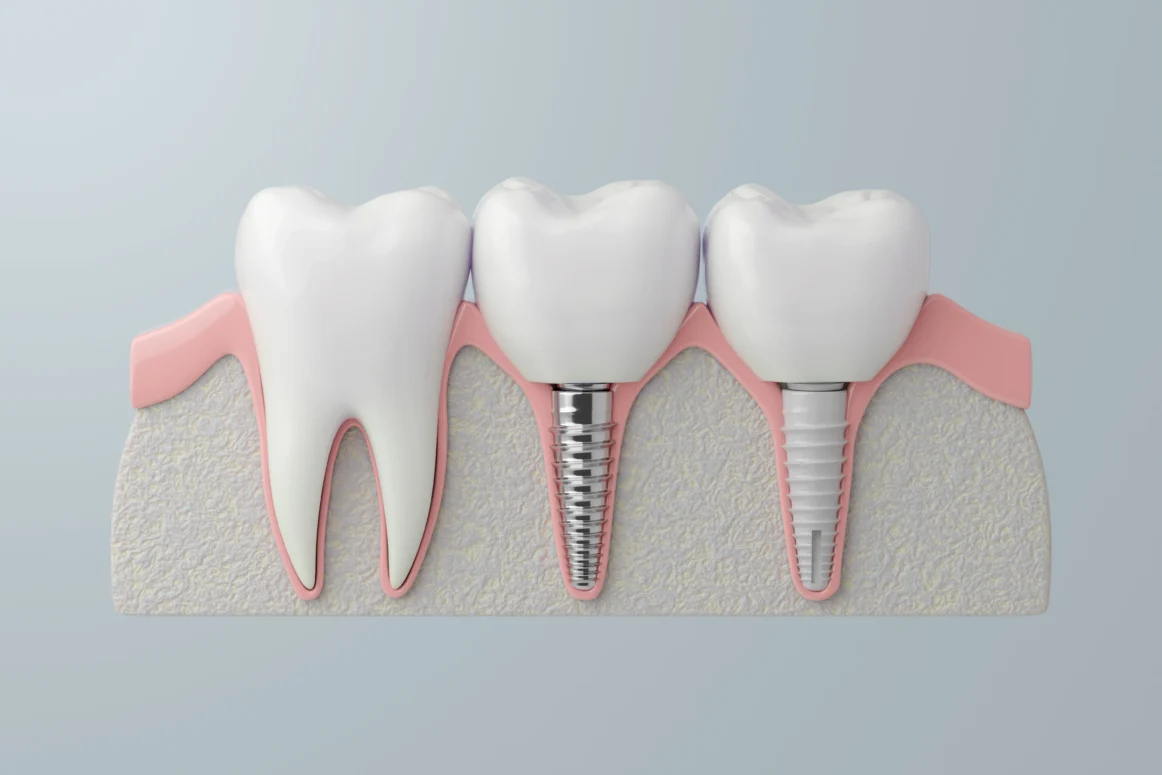
A titanium post — sized roughly like a natural tooth root — placed surgically into the jawbone. Over three to six months, the bone grows into and around it (osseointegration). Once that fusion is confirmed, a porcelain crown is attached on top, matched to the shape and shade of your surrounding teeth.
The result functions like a natural tooth. The crown absorbs bite force. The root stimulates the bone. Adjacent teeth don’t drift. Most people around you won’t know it’s there — and after a few months, you probably won’t either.
Titanium is used specifically because it’s biocompatible. Non-toxic, non-allergenic, doesn’t interact with surrounding tissue. At DentSpa we use Straumann and Nobel Biocare implant systems — both Swiss-manufactured, both with decades of clinical data behind them. These are the same systems you’d find in London, Paris, or New York.
Am I actually a candidate?
Probably, but it depends on a few things worth knowing about.
- Bone volume. The implant needs sufficient bone to anchor into. If you’ve had a gap for a while, some bone loss has almost certainly occurred. Whether that’s enough to be a problem depends on how much — and that’s what a 3D CBCT scan tells us. If the bone isn’t sufficient, bone grafting can rebuild it. It adds time, but it makes implants possible in cases that would otherwise be ruled out.
- Gum health. Active gum disease needs to be treated first. Placing an implant into inflamed tissue is asking for complications.
- General health. Uncontrolled diabetes and certain medications can slow healing and affect integration. Most conditions are manageable with the right protocols — but they need to be disclosed before treatment planning, not after.
- Smoking. Not a disqualifier. But healing takes longer and failure rates are higher. Worth discussing honestly before committing.
- Missing all or most teeth? Individual implants aren’t the only option. All-on-4 treatment uses four strategically placed implants to support a full fixed arch — a permanent, stable solution typically completed in a single surgical appointment.
What does the procedure actually involve?
- Before anything: A 3D cone beam CT scan. This maps the jaw in three dimensions — bone density, nerve location, the exact geometry where each implant will go. Without it, placement is guesswork. With it, we can plan the surgery to the millimetre and avoid complications before they happen.
- The surgery itself: Local anaesthesia, a small incision, the implant drilled into position. Most patients say it was less uncomfortable than they expected. One to two hours depending on how many implants are placed.
- Osseointegration: The implant is left alone for three to six months. A temporary restoration can be placed during this time. This isn’t a delay — it’s the process. The bone is fusing with the titanium post. Rushing it produces failures.
- Final crown: Once integration is confirmed, the custom porcelain crown is fabricated and attached. This is the last appointment.
- For patients travelling from abroad, DentSpa structures treatment across two visits. The first covers assessment and placement. The second, months later, covers the final crown. Our coordination team handles accommodation, transfers, and scheduling built around your travel.
How long do implants last?
A 2024 meta-analysis published in Clinical Oral Investigations — the first to systematically analyse 20-year implant survival rates — reported survival rates of 88–92% at the 20-year mark across prospective and retrospective studies. The titanium post itself rarely fails; most long-term issues relate to the crown or surrounding gum tissue, both of which are manageable.
The practical answer is: with proper care, decades. Maybe a lifetime.
Maintenance isn’t complicated — brush, floss around the implant, attend routine check-ups. No special equipment, no adhesives, no dietary restrictions beyond common sense.
Why is the cost so different in Turkey?
A full-mouth implant treatment at a private UK clinic runs between £25,000 and £35,000. Comparable treatment in Istanbul is a fraction of that.
The materials aren’t different. The Straumann and Nobel Biocare systems we use here are identical to those used in UK clinics. The imaging equipment, the surgical protocols, the implant brands — all the same. What’s different is operating cost. Rent, salaries, overhead — all lower in Istanbul than in London or Paris. Those savings pass directly to the patient.
DentSpa was awarded Best Dental Odontology Clinic in Europe in 2024. The evaluation criteria included technology implementation, complex case outcomes, and patient satisfaction — not pricing. We’re not competing on cost. Cost just happens to be lower here.
When should you stop waiting?
If it’s been more than three months since an extraction, bone loss has started. If you have a heavily restored tooth your dentist has mentioned extracting, planning for an implant now — before the extraction — means you can move directly to placement rather than waiting through a healing period afterward.
The window for a straightforward procedure closes gradually. It doesn’t disappear, but it gets more complicated.
Talk to our team before deciding anything
Our patient coordinators speak English, French, Arabic, Spanish, Russian, Italian, and German. A consultation is free. You’ll get a clear picture of your specific situation — including whether you need any preparation, what the timeline looks like, and what the full cost would be — before committing to anything.
Sources
- Kupka JR, et al. How far can we go? A 20-year meta-analysis of dental implant survival rates. Clinical Oral Investigations. 2024;28:541. doi:10.1007/s00784-024-05929-3
- Moraschini V, et al. Evaluation of survival and success rates of dental implants reported in longitudinal studies with a follow-up period of at least 10 years. International Journal of Oral and Maxillofacial Surgery. 2015;44(3):377–388. doi:10.1016/j.ijom.2014.10.023
- Buser D, et al. Long-term stability of osseointegrated implants in augmented bone. Clinical Oral Implants Research. 2011;22(12):1279–1285. doi:10.1111/j.1600-0501.2010.02103.x
- Gupta R, et al. Dental implants. In: StatPearls. StatPearls Publishing, 2023. PMID: NBK470448
- Jain S, et al. Evaluation of survival rates of dental implants and the risk factors: A retrospective follow-up study. Cureus. 2024;16(3):e55360. PMC10982840
- NHS. Dental implants. National Health Service, UK.














 70%
70% 

